Proton Pump Inhibitors and Antifungals: Managing Absorption and Efficacy
 Apr, 11 2026
Apr, 11 2026
PPI & Antifungal Interaction Checker
Select an antifungal medication to see how it interacts with Proton Pump Inhibitors (PPIs) like omeprazole or esomeprazole.
Recommended Strategy:
Quick Summary
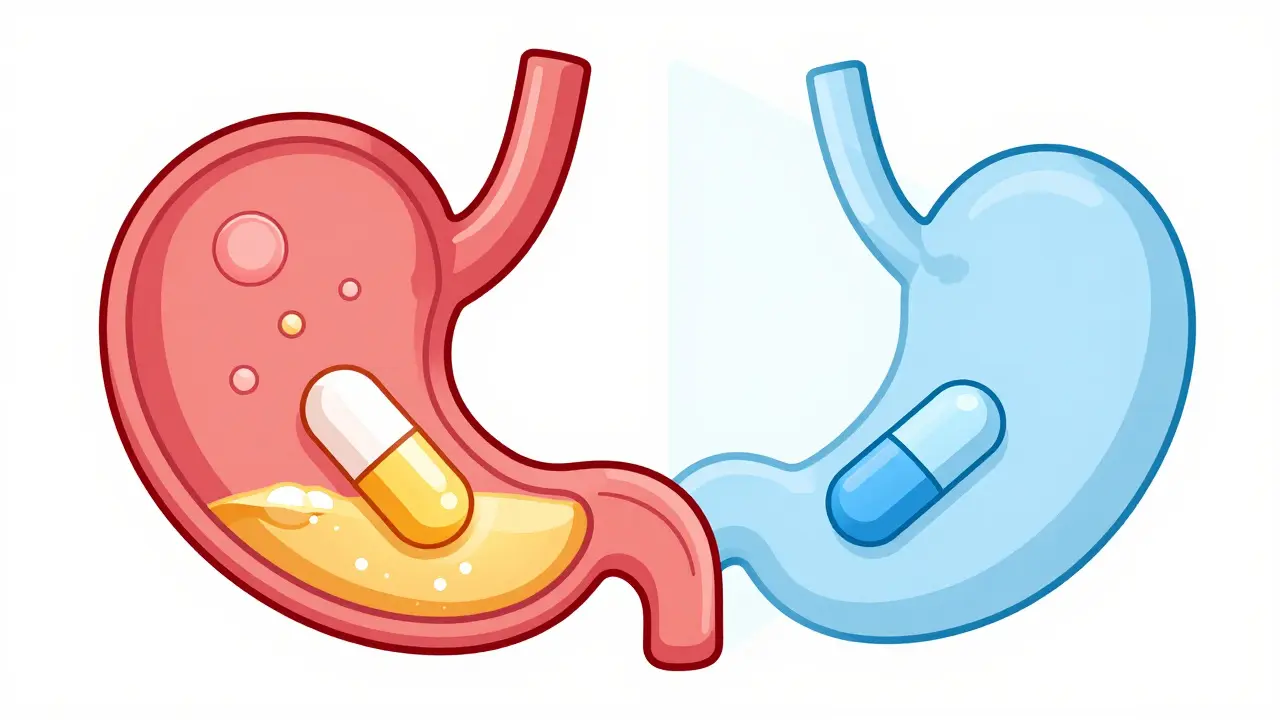
- PPIs raise stomach pH, which can block the absorption of pH-dependent antifungals like itraconazole and ketoconazole.
- Fluconazole is generally unaffected by stomach acidity and remains a safer bet when using PPIs.
- Some PPIs can actually help azoles work better against resistant Candida by inhibiting fungal pumps.
- Metabolic interactions via the CYP450 system can either increase or decrease drug levels in the blood.
- Proper timing and therapeutic drug monitoring are essential to avoid subtherapeutic dosing.
The pH Problem: Why Your Stomach Acid Matters
To understand why Proton Pump Inhibitors-like Prilosec (omeprazole) or Nexium (esomeprazole)-interfere with antifungals, you first have to look at how they work. PPIs bind to the H+/K+ ATPase pump in the stomach, effectively shutting down acid production. This shifts the gastric pH from a highly acidic 1.5-2.5 up to a more neutral 4-6. For many drugs, this is fine. But for certain azole antifungals, acid is the key to unlocking the door. Drugs like itraconazole and ketoconazole are "acid-labile," meaning they need a low-pH environment to dissolve and be absorbed by the body. When the stomach is too alkaline, these drugs simply don't dissolve. In fact, a 2023 study in JAMA Network Open found that co-administering these two classes can slash the absorption of itraconazole by a staggering 60%. If 60% of your medication never hits your bloodstream, you aren't treating an infection-you're just giving the fungus a chance to mutate.Not All Antifungals Are Created Equal
It is a common mistake to assume all azoles behave the same way. In reality, the interaction depends entirely on the specific chemical structure of the antifungal. Fluconazole, for example, is highly water-soluble. Because it doesn't rely on stomach acid to dissolve, its bioavailability stays around 90% regardless of whether you are taking a PPI. This makes it the gold standard for patients who cannot stop their acid-reflux medication. Voriconazole presents a different riddle. It doesn't have the same absorption issues as itraconazole, but it clashes with PPIs in the liver. Specifically, PPIs like pantoprazole can inhibit the enzymes responsible for breaking down voriconazole, which can actually lead to higher-than-intended levels of the drug in the system. While higher levels might sound like a win, too much voriconazole can lead to toxicity, requiring a 25-50% dose adjustment based on blood tests.| Antifungal | Absorption Impact | Metabolic Impact | Clinical Risk |
|---|---|---|---|
| Itraconazole | Severe Reduction (60% AUC loss) | Moderate | Treatment Failure |
| Ketoconazole | Severe Reduction | Moderate | Subtherapeutic Levels |
| Fluconazole | Negligible | Low (mostly affects other drugs) | Minimal |
| Voriconazole | Low | High (Reduced Clearance) | Drug Toxicity |
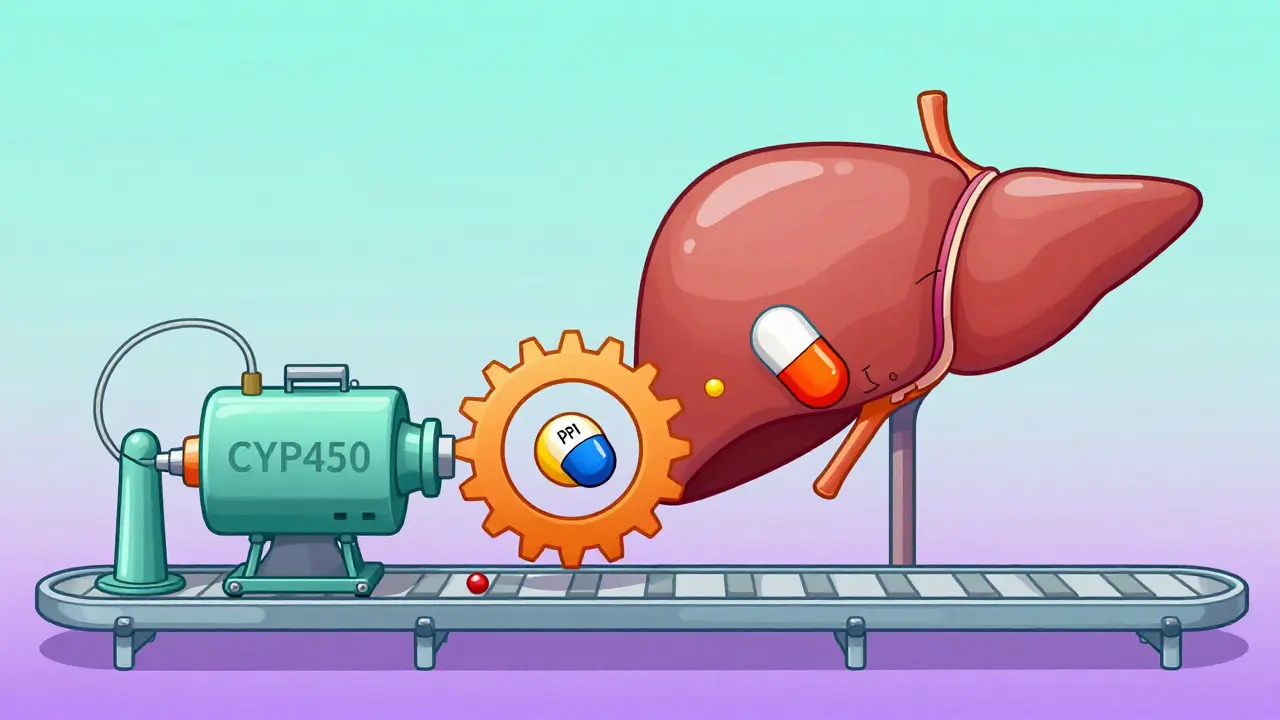
The Liver Connection: The CYP450 Battle
Beyond the stomach, these drugs fight for control in the liver. Both PPIs and azoles interact with the Cytochrome P450 (CYP) enzyme system, which is the body's primary machinery for detoxing medications. Most systemic azoles are heavily dependent on the CYP3A4 enzyme for clearance. If a PPI interferes with this pathway, the antifungal stays in the body longer. Conversely, fluconazole is a potent inhibitor of CYP2C9. This means if you're taking fluconazole along with other medications (like blood thinners), the fluconazole can block the breakdown of those other drugs, potentially leading to dangerous complications. It's a bidirectional street where one drug can either mask the presence of another or amplify its effects to a dangerous degree.The Paradox: When PPIs Actually Help
Here is where things get weird. While we've spent a lot of time talking about how PPIs ruin absorption, new research suggests they might actually make antifungals more powerful once they *do* get into the system. A groundbreaking 2024 study highlighted a mechanism involving the fungal plasma membrane ATPase (Pam1p). Essentially, some PPIs, like omeprazole, may inhibit the pumps that fungi use to eject drugs from their own cells. By "locking the doors," the PPI allows the antifungal to stay inside the fungus longer. In lab tests against resistant Candida glabrata, this synergy reduced the minimum inhibitory concentration (MIC) of fluconazole by 4 to 8 fold. This is a total pivot in how we view these drugs; we are moving from seeing PPIs as just a hurdle to seeing them as potential "adjuvants" that could help us fight drug-resistant yeast infections.
Clinical Workarounds and Safety Protocols
So, what happens if a patient absolutely needs both a PPI and a pH-dependent antifungal? You can't just hope for the best. Clinical protocols from institutions like the Mayo Clinic and UCSF suggest specific strategies to minimize the damage:- Strategic Timing: For itraconazole, the drug should be administered at least 2 hours before the PPI. For ketoconazole, a wider gap of 4 to 6 hours is recommended, though this only partially restores absorption.
- Therapeutic Drug Monitoring (TDM): This is non-negotiable for voriconazole and itraconazole. Doctors must check trough concentrations (the lowest level of the drug in the blood before the next dose) to ensure they are within the therapeutic window (e.g., 0.5-1.0 μg/mL for itraconazole).
- Switching Agents: In many cases, the safest route is to switch to an antifungal that isn't pH-dependent, such as the echinocandins class, which avoids the gastric pH issue entirely.
Looking Ahead: The End of pH Dependence?
We are likely entering the final era of this specific drug-drug struggle. Researchers are currently developing "pH-independent" formulations. For instance, a submicron particle version of itraconazole (SUBA-itraconazole) has shown 92% bioavailability regardless of whether the stomach is acidic or alkaline. Once these formulations hit the market, the need to carefully time doses or switch to less effective alternatives will vanish. Until then, the mantra for clinicians remains: check the pH, monitor the blood, and when in doubt, switch the antifungal.Can I take omeprazole and fluconazole together?
Yes, generally. Fluconazole is highly water-soluble and does not require stomach acid for absorption, so its efficacy is not reduced by the increase in pH caused by omeprazole. However, you should still consult a doctor regarding potential liver enzyme interactions.
Why is itraconazole specifically affected by PPIs?
Itraconazole is a pH-dependent drug. It requires a highly acidic environment (low pH) to dissolve into a solution that the body can absorb. PPIs raise the stomach pH, preventing the drug from dissolving, which can reduce its absorption by up to 60%.
What is a "black box warning" in this context?
The FDA added a black box warning to itraconazole in 2023 to alert providers that using it with PPIs is contraindicated because it significantly lowers the concentration of the antifungal in the plasma, risking treatment failure.
Do PPIs always make antifungals worse?
Not necessarily. While they hurt absorption for some, recent research suggests PPIs can actually act as adjuvants. By inhibiting the Pam1p pump in fungi, they may help antifungals like fluconazole stay inside the fungal cell longer, potentially overcoming some forms of drug resistance.
What should I do if I must take both a PPI and a pH-dependent antifungal?
Under medical supervision, you should separate the dosing. Typically, the antifungal is taken several hours before the PPI. Your doctor may also perform therapeutic drug monitoring (TDM) via blood tests to ensure the antifungal levels are high enough to be effective.