H2 Blockers and Their Critical Interactions with Antivirals and Antifungals
 Mar, 21 2026
Mar, 21 2026
When you take an H2 blocker like famotidine or cimetidine for heartburn or ulcers, you might not think it affects your antifungal or antiviral meds. But it does - and sometimes in dangerous ways. These drugs don’t just calm stomach acid; they can sabotage the effectiveness of life-saving treatments for infections like fungal pneumonia or HIV. Understanding how H2 blockers interact with antivirals and antifungals isn’t optional - it’s essential to avoid treatment failure, hospitalization, or worse.
How H2 Blockers Work (And Why It Matters)
H2 blockers, or histamine H2-receptor antagonists, reduce stomach acid by blocking histamine from signaling your stomach to produce more acid. The most common ones still in use are famotidine (a medication used to treat GERD and peptic ulcers), cimetidine (an older H2 blocker with significant drug interaction risks), and nizatidine (a less commonly used H2 blocker with moderate interaction potential). Ranitidine was pulled from the market in 2020 after contamination with NDMA, a probable carcinogen.
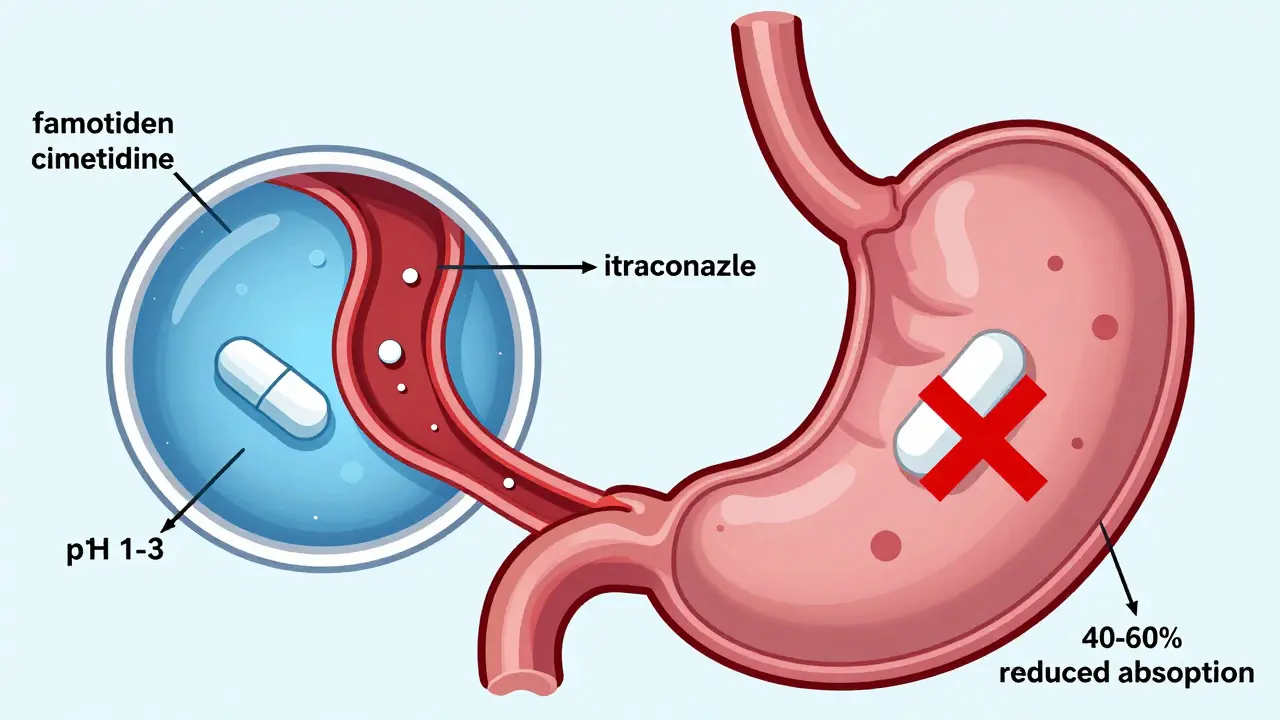
Normal stomach acid has a pH of 1-3. H2 blockers raise that to 4-6. That sounds harmless - until you realize some drugs need that strong acid to dissolve and get absorbed. If your stomach is too alkaline, those drugs just pass through without doing their job.
Why Antifungals Are Especially Vulnerable
Not all antifungals are affected the same way. The big problem lies with azole antifungals - especially itraconazole (a broad-spectrum antifungal used for invasive fungal infections). Itraconazole tablets require a highly acidic environment to dissolve. Studies show that when taken with an H2 blocker, its absorption drops by 40-60%. That means your body gets less than half the dose you took - and the infection might not just survive, it might spread.
Fluconazole, on the other hand, is water-soluble and doesn’t care about pH. It absorbs just fine even with famotidine. Voriconazole and posaconazole are in between - they’re affected, but not as badly as itraconazole. Isavuconazole is the newest and most forgiving; it has fewer interactions because it doesn’t rely heavily on CYP enzymes or stomach acid.
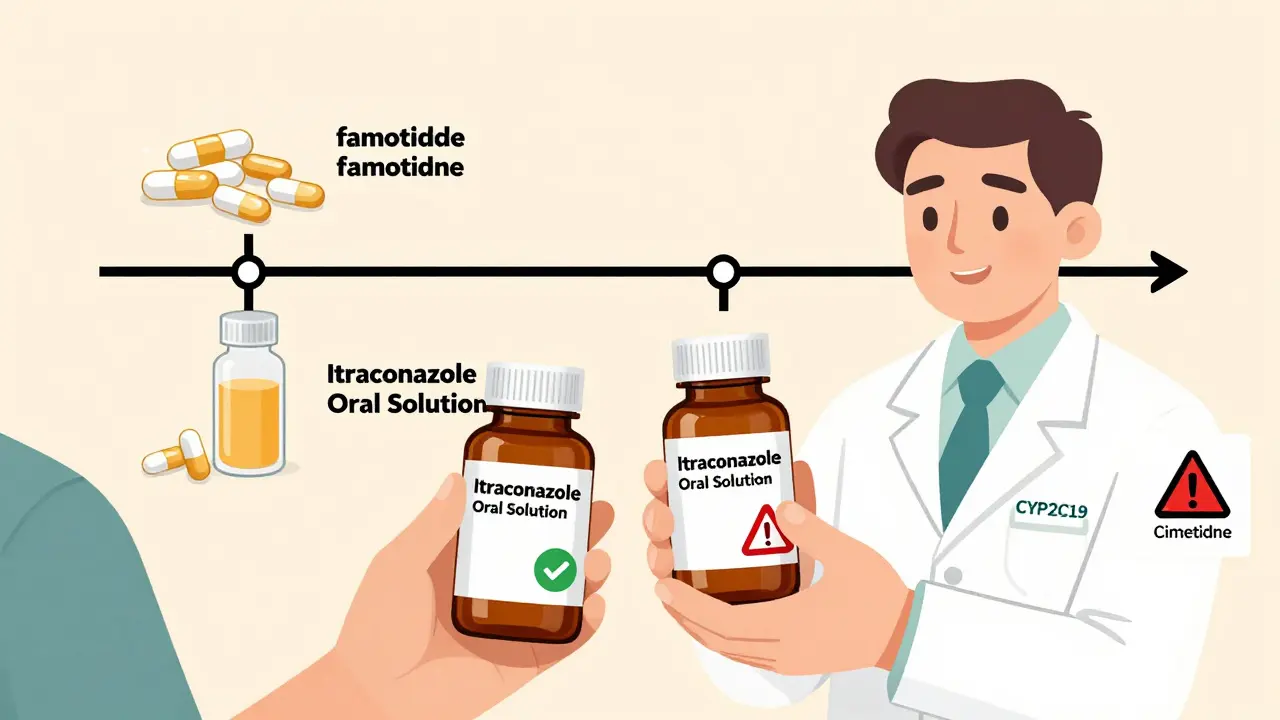
The FDA recommends separating itraconazole and H2 blockers by at least two hours. But here’s the catch: if you’re taking itraconazole tablets, even that might not be enough. The oral solution form - which contains citric acid - is much more reliable. Many patients don’t know this distinction. Pharmacists report that nearly half of patients on itraconazole aren’t told which form to use or how to time it with acid reducers.
Antivirals Don’t Escape Either
Antivirals like atazanavir (an HIV protease inhibitor) are also pH-dependent. When taken with famotidine, atazanavir exposure drops by up to 77%. That’s not a small drop - it’s enough to cause viral resistance. The FDA explicitly says: take atazanavir at least two hours before the H2 blocker.
Dasatinib, used for certain leukemias and sometimes off-label for antiviral effects, shows similar issues. Other antivirals like rilpivirine and erlotinib also suffer reduced absorption with acid suppression. A 2022 FDA review found that 68% of antiviral labels included warnings about acid-reducing agents - and H2 blockers were named in nearly a third of those cases.
What makes this worse is that many patients are on multiple medications. Someone with HIV might also get antifungals for a yeast infection. A transplant patient might be on voriconazole for aspergillosis and famotidine for stress ulcers. These combinations aren’t rare - they’re common. And without clear guidance, they’re risky.
Cimetidine Is the Worst Offender
Not all H2 blockers are equal. cimetidine (an H2 blocker with strong cytochrome P450 enzyme inhibition) is the most dangerous. It blocks key liver enzymes - CYP1A2, CYP2C9, CYP2C19, and CYP2D6 - that break down many drugs. This means it doesn’t just mess with absorption; it can cause toxic buildup.
For example, cimetidine can raise voriconazole levels by 40%, increasing the risk of liver damage and vision problems. Voriconazole can also slow cimetidine’s breakdown, leading to dizziness, confusion, or even gynecomastia. This two-way interaction is rare with other H2 blockers.
Famotidine and nizatidine don’t inhibit CYP enzymes. That’s why they’re now the go-to choices when acid suppression is needed alongside antifungals or antivirals. A 2023 IQVIA analysis showed that 92% of patients switched from cimetidine to famotidine when starting azole antifungals.
What Clinicians Should Do
There’s no one-size-fits-all fix, but there are clear steps:
- Check the drug label. Every antiviral and antifungal has a section on drug interactions. Look for phrases like “avoid concurrent use” or “separate by 2 hours.”
- Prefer famotidine over cimetidine. If you need an H2 blocker, use famotidine. It’s safer, just as effective, and doesn’t interfere with liver enzymes.
- Time it right. For itraconazole tablets, give the antifungal at least 2 hours before the H2 blocker. For atazanavir, take it 2 hours before the H2 blocker. For voriconazole, monitor blood levels if used with cimetidine.
- Use alternatives when possible. For itraconazole, the oral solution is more reliable. For antifungals, consider isavuconazole - it has fewer interactions and is non-inferior to voriconazole in treating invasive aspergillosis.
- Educate patients. A 2022 survey found only 43% of hospital pharmacists consistently gave timing instructions to patients on itraconazole. That’s too low. A simple verbal reminder can prevent treatment failure.
What’s Changing Now
The FDA is pushing for clearer labeling. By late 2026, all drugs affected by gastric pH must include specific timing instructions on their labels. That’s a big step forward.
Researchers are also testing new formulations. One trial (NCT04821542) is looking at lipid-based itraconazole that absorbs even in higher pH. If it works, it could eliminate this interaction entirely.
Meanwhile, the American Society of Health-System Pharmacists (ASHP) recommends using H2 blockers instead of proton pump inhibitors (PPIs) when possible - because PPIs suppress acid for 24+ hours, while H2 blockers wear off in 6-12 hours. That gives you a window to safely give the antifungal or antiviral.
Bottom Line
H2 blockers aren’t harmless. They’re powerful enough to make antivirals and antifungals fail - and that can kill. Cimetidine is risky. Famotidine is safer. Timing matters. Formulation matters. And most of all, awareness matters.
If you’re on an antifungal or antiviral and you take heartburn meds, ask: Is this the right H2 blocker? Am I taking it at the right time? Is there a better option? Don’t assume it’s safe - check.
Can I take famotidine with fluconazole?
Yes. Fluconazole is highly water-soluble and doesn’t need stomach acid to absorb. Famotidine doesn’t interfere with its effectiveness. This combination is generally safe and commonly used.
Is cimetidine safe with voriconazole?
No. Cimetidine strongly inhibits the CYP2C19 enzyme, which breaks down voriconazole. This can cause voriconazole levels to spike by up to 40%, raising the risk of liver damage and visual disturbances. Avoid combining them. If you must use both, monitor blood levels closely and consider switching to famotidine.
Why is itraconazole so sensitive to stomach acid?
Itraconazole tablets are poorly soluble in water and require an acidic environment to dissolve. When stomach pH rises above 3 - which happens with H2 blockers - the tablets don’t break down properly. As a result, absorption drops by 40-60%. The oral solution form contains citric acid, which helps it dissolve regardless of pH.
Can I take an antacid instead of an H2 blocker?
Antacids (like Tums or Maalox) can raise stomach pH even more quickly and intensely than H2 blockers. They’re even more likely to reduce absorption of pH-dependent drugs. If you need acid suppression, H2 blockers are generally preferred over antacids - but timing still matters. Always follow the specific instructions for your medication.
What should I do if I’m on atazanavir and need heartburn relief?
Take atazanavir at least two hours before your H2 blocker. If you’re on famotidine, that timing is usually sufficient. Avoid cimetidine entirely. If heartburn is frequent, talk to your doctor about whether you truly need acid suppression - or if lifestyle changes (like avoiding spicy food or eating earlier) might help instead.
Amber Gray
March 22, 2026 AT 21:55Danielle Arnold
March 23, 2026 AT 18:05James Moreau
March 24, 2026 AT 13:18J. Murphy
March 24, 2026 AT 23:55Jesse Hall
March 26, 2026 AT 07:07Donna Fogelsong
March 27, 2026 AT 23:01Sean Bechtelheimer
March 29, 2026 AT 13:53Seth Eugenne
March 30, 2026 AT 04:05rebecca klady
March 30, 2026 AT 20:43Namrata Goyal
March 30, 2026 AT 22:57